Menopause and perimenopause aren’t just about hot flashes and mood swings hitting you at the worst possible time. It is…

Menopause and perimenopause aren't just about hot flashes and mood swings hitting you at the worst possible time. It is a special period when your body undergoes major changes, not the ovaries but the intestines are at the centre of this process! Gut health and hormones during menopause are tightly connected. It's amazing how our bodies work, isn't it?
Studies show that decreased estrogen levels change the gut microbiome or bacteria in the gut, which causes changes in digestion, mood, sleep and even bone health. Incredibly, the gut plays a huge role in hormone metabolism! Understanding the connection between gut health and hormones during perimenopause and menopause can help you take control of your symptoms naturally. How? If changes in hormones influence our microbiome – can the change of microbiome also influence our hormones? Let's dive into this hot topic and learn practical steps to help us maintain and even improve health during this transitional period. Read here more about how to manage your hormonal balance during Menopause
Why Gut Health and Hormones Matter in Menopause
The hormonal changes during menopause, specifically the decrease in estrogen levels, significantly impact bacteria in your gut and vagina (sources 1, 2). Estrogen affects the diversity and composition of gut bacteria, changing how your body digests and assimilates food, responds to illness, and maintains overall health.
Menopause brings a new hormonal balance that we used to think of as an imbalance. But it's certainly a new hormonal balance, and if it wasn't, women would just die after menopause. Life expectancy studies show that Japanese women who do not take hormone therapy after menopause have the longest life expectancy in the world and their health during this period is stronger than their counterparts from developed countries (source).
So, menopause is a period in which our body adapts to a new hormonal order, and this undoubtedly entails changes in the composition and balance of our gut bacteria. They simply have to adapt to the new order. If we delay or resist this transformation, because we are not ready to live the new life, we are assured of gut reactions such as abdominal bloating, irregular emptying and inflammation. There is a battle going on in our gut and we are reaping the benefits.
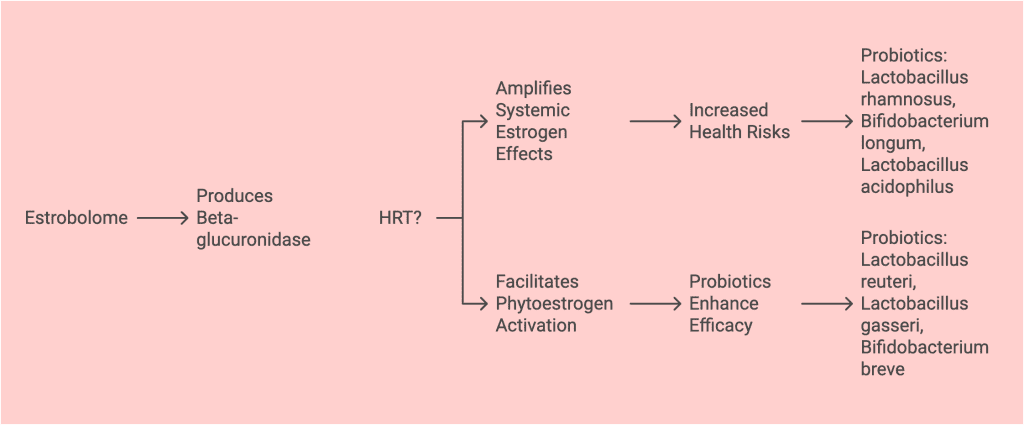
Among the gut bacteria, there is a special subgroup known as estrobolome – which plays a critical role in regulating estrogen metabolism. Estrobolome produces the enzyme beta-glucuronidase, which helps process and maintain optimal estrogen levels. If you don't “buddy up” to estrobolom its composition gets disrupted, and menopausal symptoms such as hot flashes and weight gain will intensify. That's why it's important to maintain a healthy estrobolom ( and not just a diverse gut microbiome) to keep your hormones in a new balance.
Are you bothered by sudden mood swings? If so, keep in mind the gut-brain connection, or the gut-brain axis, which also emphasizes the importance of gut health during menopause. When estrogen levels drop, this “shifts” the gut-brain axis, which will lead to mood swings, anxiety and decreased mental clarity.
Gut bacteria produce neurotransmitters such as serotonin and GABA that affect our emotional state. If microbiota is unhealthy (incompatible with our needs), these neurotransmitters will be produced in lower amounts, which makes us feel blue and affect our cognitive abilities.
So changes in diet, probiotics and lifestyle changes are not whimsical, but a necessity to get through menopause and come out of it not only symptom-free but also without loss of health and improved life longevity.
The Impact of Menopause on the Gut Microbiome
What do we know about gut microbiome in menopause? The effect of estrogen on gut health is ambiguous. While it maintains the mucosal defence layer and protects against dangerous oxidants (source 1, 2), it also disrupts the integrity of the intestinal wall and stimulates the growth of potentially unfavourable microbiota (source). Decreased estrogen levels seriously affect the gut microbiome. It can lead to a condition called dysbiosis – or disruption of our individual diversity and balance of microbes in the gut that are used to ensure optimal health (source).
Estrogen is not particularly healthy for gut health or general health because it disrupts the integrity of the gut wall (source). Looks like our bodies learn to adapt to these conditions through the cyclical rise and fall of estrogen during the reproductive period.

When estrogen levels decrease, the likelihood of a “leaky gut” should also decrease. The decline in estrogen also causes a decrease in the diversity of microbes in the gut, which is linked to various health problems). If you fail to support gut health, opportunistic and potentially harmful bacteria can begin to thrive. This leads to digestive problems: abdominal bloating and constipation, systemic inflammation and increased menopause symptoms such as joint pain and fatigue.
The Role of Beta-Glucuronidase
The enzyme beta-glucuronidase is produced by certain gut bacteria as part of the estrobolome. This enzyme helps regulate estrogen recycling, returning water-soluble estrogen that has transformed in the liver to its original, fat-soluble form. This allows active estrogen to re-enter the bloodstream (source ).
How beta-glucuronidase activity will affect you depends on what level of estrogen is in your body and how your cells respond to it.
If you're healthy and not using HRT, beta-glucuronidase can help you maintain your estrogen levels, recycling used estrogen. If, however, you use HRT or have genetic mutations in your liver function that might lead to estrogen-dependent disease, beta-glucuronidase may work against you.
Dysbiosis in the gut makes it difficult for your body to absorb nutrients, which can lead to a decrease in important vitamins and minerals like calcium and magnesium, which are essential for strong bones during menopause. Because of these nuances, customized menopause solutions especially regarding diet and supplements become incredibly important.
General Strategies to Improve Gut Health During Menopause
Diet
Addressing the issue with beta-glucuronidase and improving gut health during menopause starts with thoughtful dietary choices. Fiber-rich foods such as oats, seeds, lentils and leafy greens become vital to maintaining gut microbial diversity and healthy digestion.
Fiber acts as a prebiotic, supporting beneficial gut bacteria. Phytoestrogens found in soy and flaxseed provide additional hormonal support by modulating estrogen levels. They mimic the mild estrogenic effect but can also protect our cells from its excessive levels, which is crucial if you have a family history of female cancers.
These dietary changes not only support the microbiome, but also contribute to overall well-being by reducing abdominal bloating, increasing regularity, and alleviating symptoms such as hot flashes.
Probiotics and prebiotics
Probiotics and prebiotics are powerful tools for restoring and maintaining a balanced gut microbiome. Not all of them, but certain types.
Lactobacillus and Bifidobacterium, have been shown to help metabolize estrogen, support estrobolom, help reduce inflammation and improve digestion, which is a common problem during menopause.
Prebiotic foods such as flax, garlic, onions and bananas provide the nutrients needed to fuel these beneficial bacteria, increasing their effectiveness. Combining probiotics with fibre creates a synergistic effect, further improving gut health and reducing menopause symptoms.
Lifestyle
Stress can disrupt the gut-brain axis, leading to an imbalance in the microbiome and exacerbating anxiety and digestive discomfort. Practising mindfulness, deep breathing, yoga or meditation helps regulate this axis, improving our psyche and gut health.
Regular exercise, surprisingly, also promotes gut microbial diversity and supports hormonal regulation. Activities such as walking, strength training or swimming not only boost mood but also improve digestion and reduce inflammation, setting the stage for better gut health and overall resilience during menopause.
The Role of Hormone Replacement Therapy (HRT)
Hormone replacement therapy (HRT), especially estrogen-containing therapy, has a significant impact on gut health and possibly restrains previous microbial diversity in the microbiome. I think it imposes a new order on the microbiome colonies of the gut and vagina. Estrogen affects estrobolome, a subset of gut bacteria responsible for estrogen metabolism.
- The use of HRT, even in transepidermal form, is known to selectively promote bacteria with beta-glucuronidase activity, which returns waste estrogen from the liver to the tissues, further increasing estrogen levels (source)
- This creates a feedback loop in which increased estrogen levels stimulate further processing of estrogen. This is very dangerous if you are at risk of developing cancer or thrombosis.
- All of these events cause further unfavourable transformation of the microbiota and amplify the negative properties of estrobolome.
HRT carries serious risks and is not suitable for everyone: women with a history of estrogen-sensitive cancer or certain cardiovascular conditions should consult a doctor. But even if your genetics are fine and you choose to go on HRT, keep in mind these risks can be greatly reduced by managing estrobolome through diet, supplements, and other lifestyle strategies.
Probiotics for Hormonal Balance
Probiotics play one of the most important roles in maintaining hormonal balance during menopause. Read here about the Best Supplements during Menopause
Which ones are right for you depends on how long you've been taking hormone therapy (and what kind), whether you have a family history of female cancer or genetic predispositions to poor estrogen transformation in the liver and your lifestyle.
Probiotics helpful with HRT:
If you decide to take HRT, combine hormone therapy with healthy habits. A diet rich in fibre, phytoestrogens and probiotics supports a healthy microbiome and complements the effects of HRT.
You will need special strains of probiotics that reduce the activity of bacteria that produce beta-glucuronidase:
- Lactobacillus rhamnosus (e.g., LGG strain):
- Promotes gut health by reducing the population of pathogenic bacteria.
- Helps reduce beta-glucuronidase activity indirectly, improving microbial balance and reducing inflammation.
- Lactobacillus acidophilus:
- Promotes a microbiome that minimizes estrogen deconjugation.
- Produces lactic acid, which lowers intestinal pH and inhibits beta-glucuronidase-producing bacteria.
- Lactobacillus plantarum:
- Reduces intestinal permeability and improves microbial balance, potentially reducing beta-glucuronidase activity.
- Bifidobacterium longum:
- Directly inhibits beta-glucuronidase activity, modulating the microbial population.
- Supports detoxification processes in the liver and intestine by promoting estrogen conjugation and excretion.
- Bifidobacterium breve:
- Enhances the integrity of the intestinal barrier and may reduce levels of harmful microbial metabolites.
- Bifidobacterium bifidum:
- Competes with beta-glucuronidase-producing bacteria to help regulate estrogen processing.
- Saccharomyces boulardii (beneficial yeast):
- Known for their anti-inflammatory properties.
- Help modulate gut microbial composition and indirectly reduce beta-glucuronidase activity.
- Streptococcus thermophilus:
- Produces metabolites that inhibit the growth of beta-glucuronidase-producing bacteria.

Probiotics helpful with phytoestrogen-based approach
If you decide to stay HRT-free and rely on phytoestrogens (e.g., from soy, flaxseed, or other plant sources), your strategy shifts to supporting beta-glucuronidase activity and phytoestrogen metabolism. This is because beta-glucuronidase enzymes are needed to deconjugate phytoestrogen metabolites in the gut, converting them into their bioactive forms (e.g., equol, enterolactone, or enterodiol). These active forms mimic estrogen and exert beneficial estrogenic effects.
Probiotics That Enhance Beta-Glucuronidase Activity
- Lactobacillus reuteri:
- Promotes metabolism of phytoestrogens like daidzein into equol.
- Supports intestinal epithelial health and estrogenic signalling.
- Lactobacillus gasseri:
- Aids in converting soy isoflavones into equol.
- Has been associated with improved estrogenic activity in postmenopausal women.
- Lactobacillus casei:
- Supports general beta-glucuronidase activity, promoting phytoestrogen bioactivation.
- Bifidobacterium breve:
- Metabolizes lignans from seeds (e.g., flaxseed) into bioactive enterolignans like enterolactone and enterodiol.
- Bifidobacterium infantis:
- Supports estrogen-like activity by enhancing the metabolism of dietary phytoestrogens.
- Lactobacillus and Bifidobacterium species that encourage the deconjugation of phytoestrogens into bioactive forms
Probiotics That Support Phytoestrogen Utilization
- Improves the gut fermentation of lignans and supports the production of enterolactone and enterodiol.
- Produces enzymes that assist in the breakdown and activation of phytoestrogens. Specific strains of these bacteria are associated with the metabolism of plant-derived phytoestrogens.
-
- Lactococcus lactis:
- Enterococcus faecium:
- Clostridium saccharogumia and Clostridium scindens
When choosing a probiotic supplement for hormonal balance, it’s essential to select clinically validated strains with proven benefits. Look for supplements that provide clear information about the specific strains included, such as Lactobacillus rhamnosus and Bifidobacterium breve, and ensure they contain an adequate number of Colony Forming Units (CFUs), typically in the range of 10-20 billion CFUs per dose, for maximum efficacy. To enhance the effects of probiotics, combine them with prebiotics—non-digestible fibres that fuel beneficial bacteria.
- Examples:
Emerging Research and Future Directions
The more we know estrobolome, the better we will learn how to influence gut bacteria, and through them, estrogen metabolism.
Research is ongoing, with a particular focus on how manipulation of the gut microbiome may improve estrogen regulation, potentially reducing menopause-related discomfort and providing protective effects for bone and heart health. All of this only reinforces the growing importance of the gut as a critical factor in menopause management, in addition to its role in digestion.
How does the strategy for managing gut health change during the menopausal transformation? The future of menopause management is increasingly leaning towards personalized approaches to gut health, and estrogen metabolite and microbiome testing plays a key role in this.
By analyzing the unique composition of your gut microbiota, we can personalize the type of probiotics, diet, and even lifestyle changes to optimize our individual hormone balance. This personalized approach has the potential to provide better management of our menopause symptoms and general health but remember, gut health varies greatly from person to person.
Conclusion:
Our gut health holds the important key to navigating menopause with balance and ease. By understanding how gut bacteria interact with hormones, we can take proactive steps like improving our diet, adding probiotics, and managing stress to support our overall well-being. Whether you choose natural remedies or complement your routine with HRT, prioritizing gut health is a game-changer. Ready to start? Take the first step by focusing on your microbiome today for a healthier, happier menopause journey!




